ABCD’s of Reducing Stroke
What is the project focus?
ACTION has been working to reduce the frequency of stroke associated with pediatric VAD care ever since it was established in 2017. Previous studies showed stroke rates in children on VADs ranged from 10% to 29% depending on device. We introduced the ABC’s of Stroke Prevention to standardize care and ultimately improve outcomes. These ABCs have dramatically decreased the rate of stroke to <12% in Berlin Heart and <5% in implantable VADs. In 2020, we organized discussion & data or commonly known as morbidity and Mortality review of all stroke events that occur in the network. We are now identifying the root causes of every stroke that occurs at every single ACTION site as a team.
To learn more, see the Project Charter.
Who is impacted?
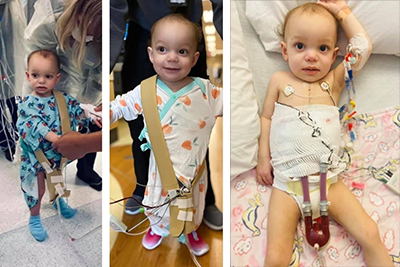
Heart failure patients implanted with a ventricular assist devices.
What are we doing to help?
- standardized anticoagulation protocol
- standardized blood pressure management protocol
- communication checklist for the bedside
- standard presentation format for every stroke that occurs in network
What data do we have?
Aggregate network stroke data, coming back soon.
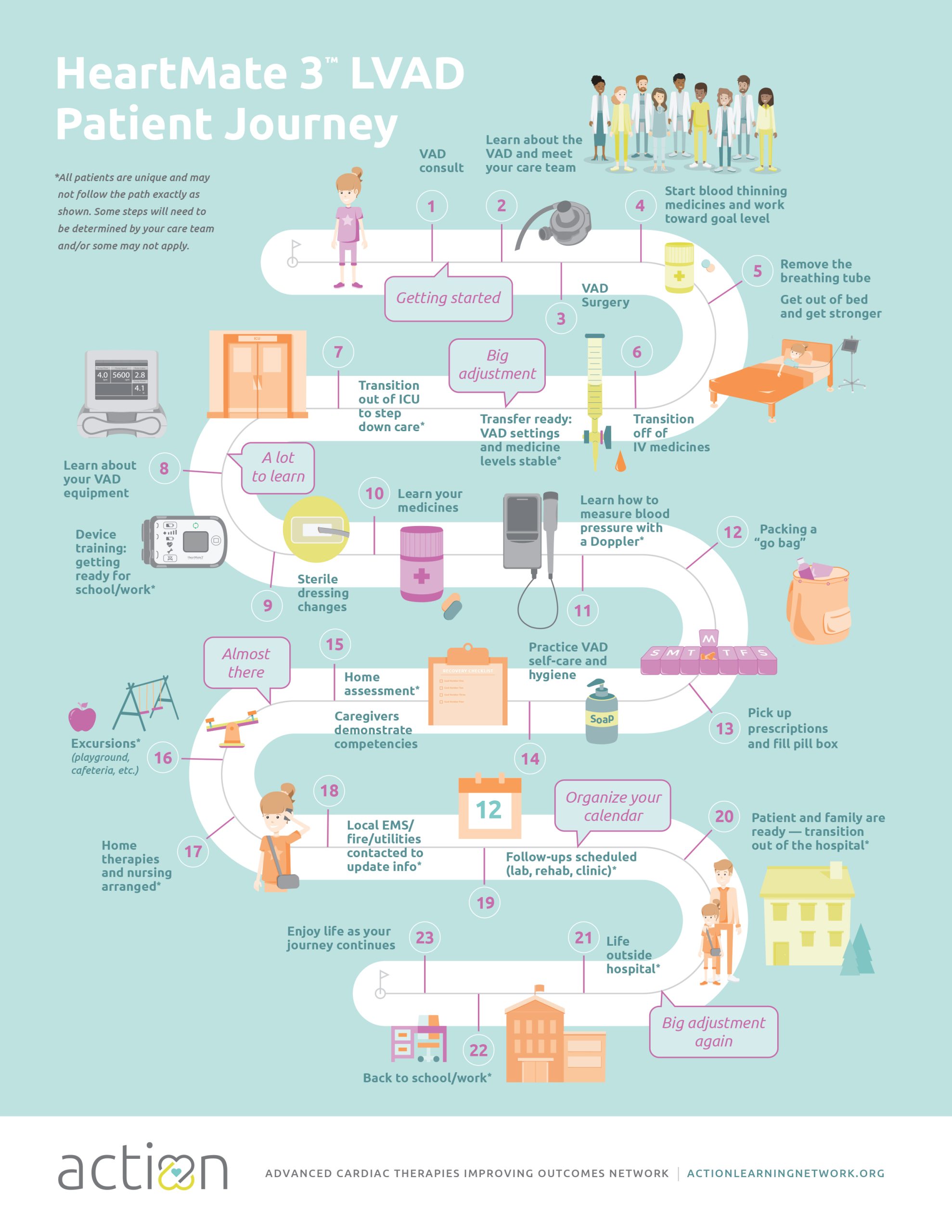
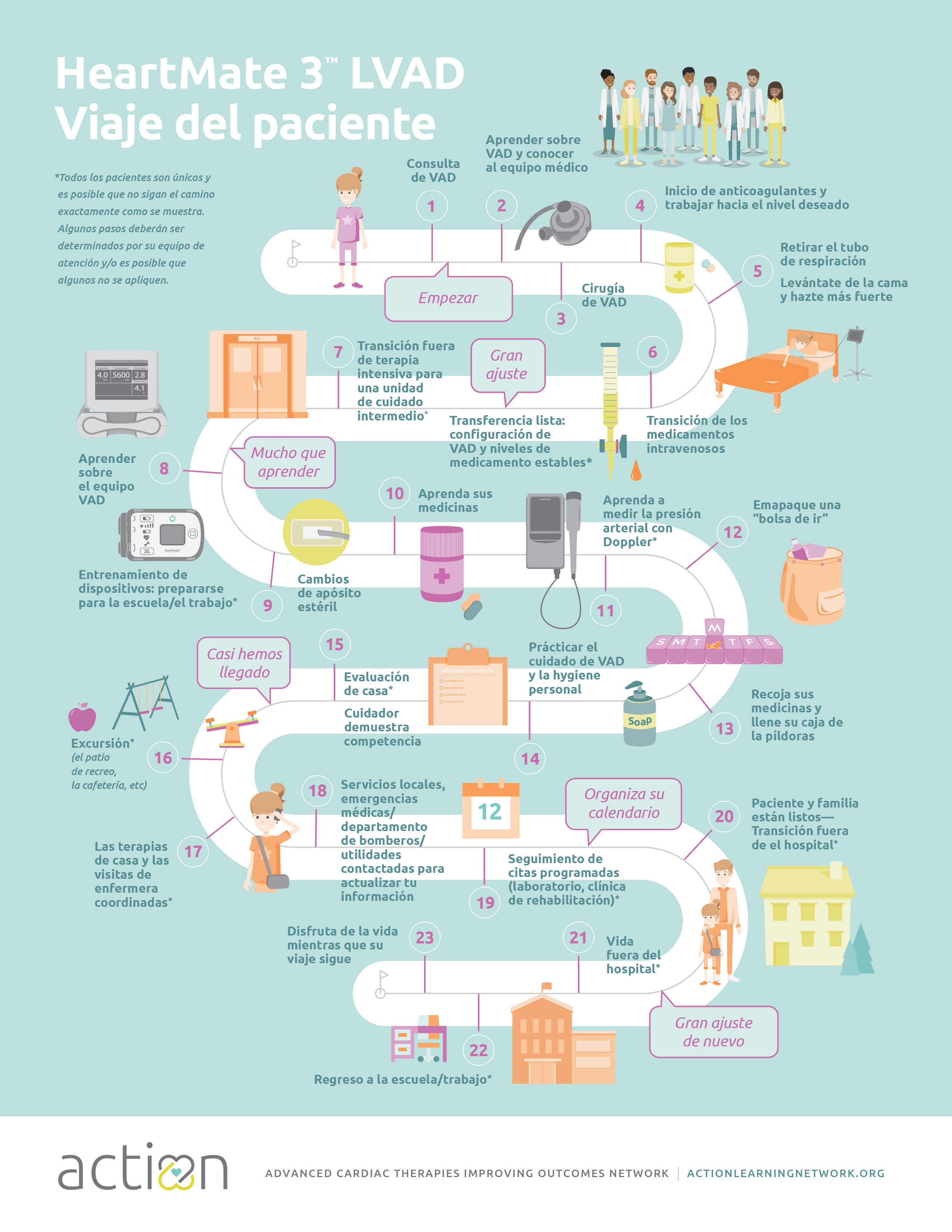
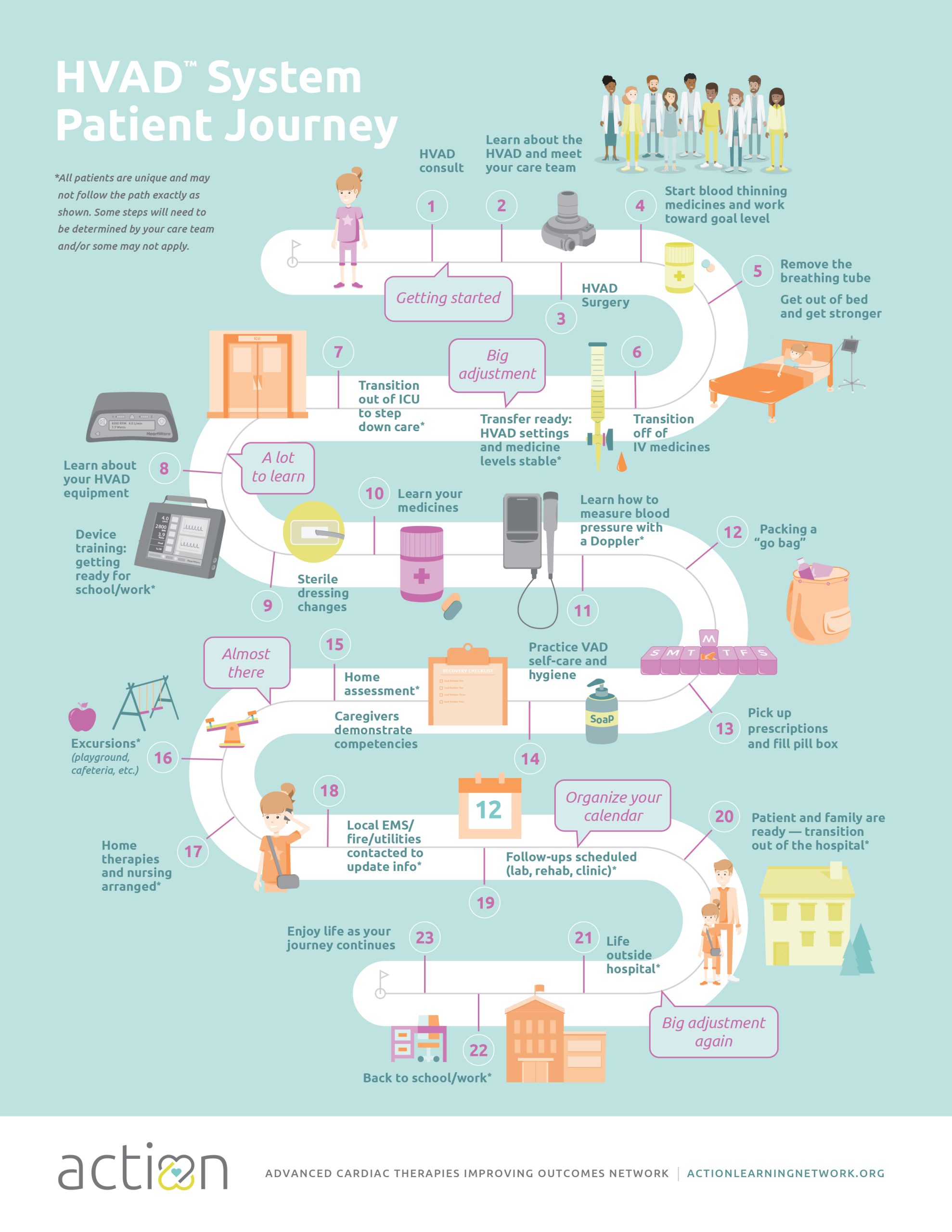
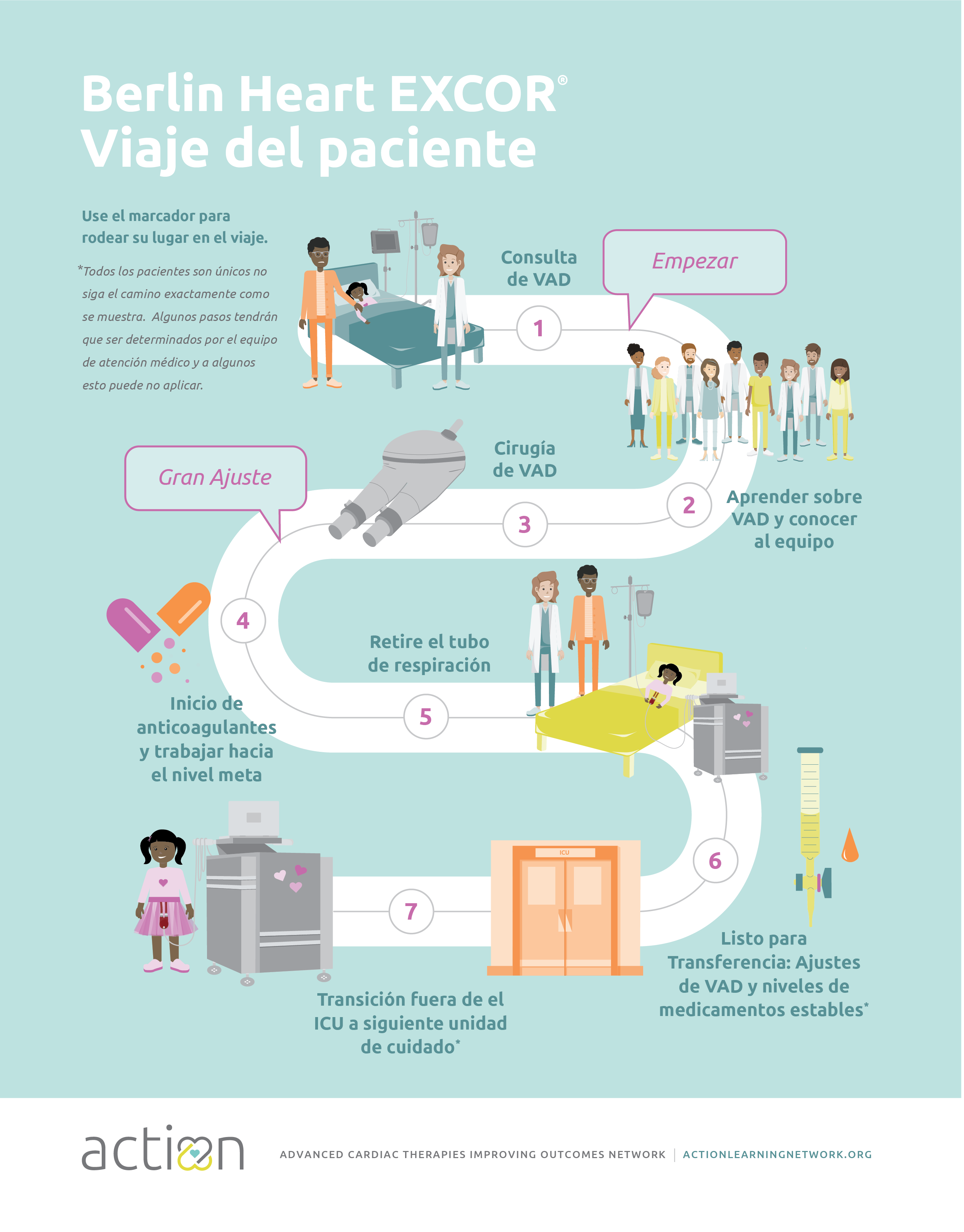
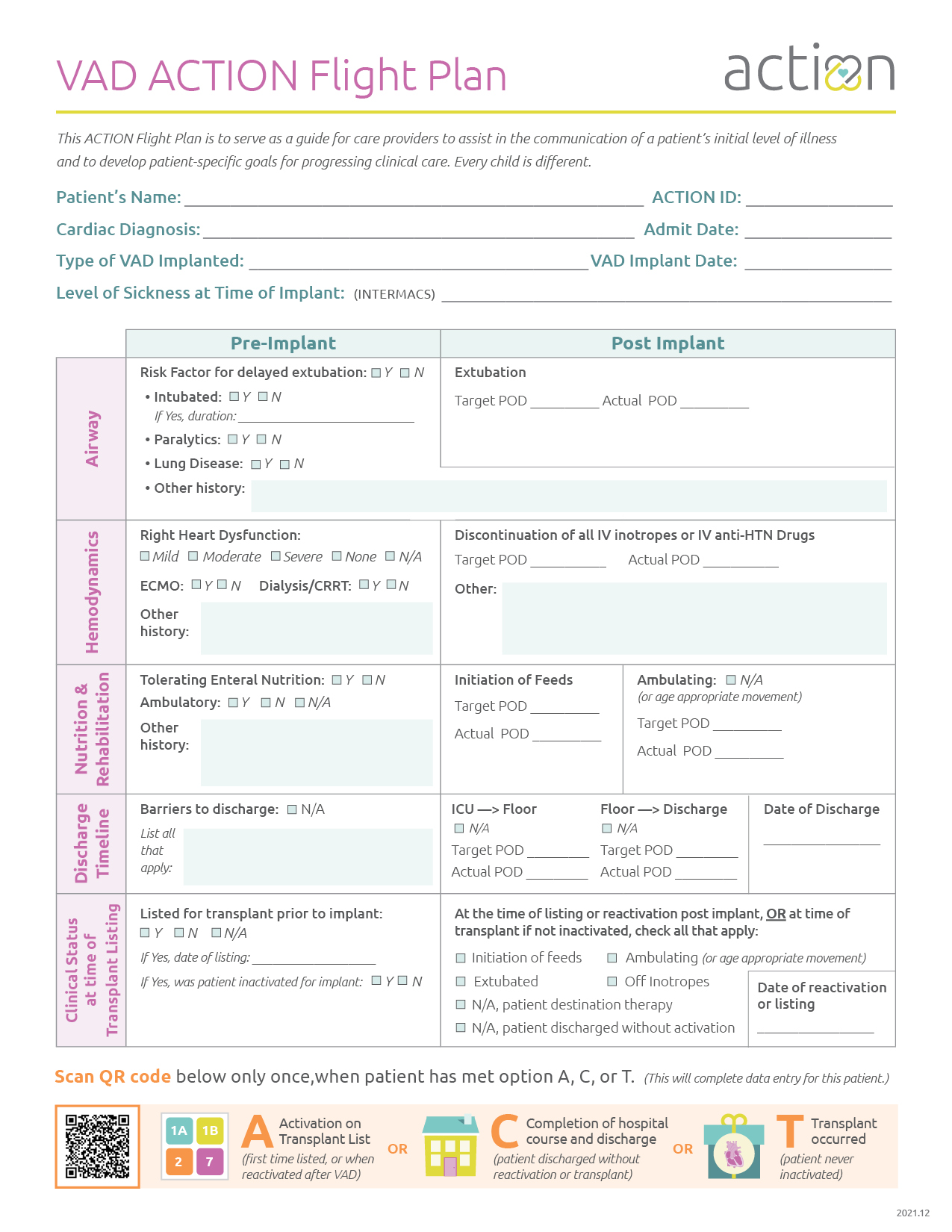
VAD Discharge & De-Escalation of Care
What is the project focus?
For over a year, we have focused on improving discharge rates for VAD patients. We found that only about 50% of pediatric patients with dischargeable VADs actually are discharged from the hospital on their VAD. We also found that 1/3 of VAD patients undergo transplant prior to discharge from the hospital, in some cases these patients may not be as strong as possible before transplant. The scope of our project has now expanded to better understand factors influencing transplant listing, specifically de-escalation of care. We are also focused on improving communication regarding the milestones of post-operative care.
Who is impacted?
Heart failure patients implanted with ventricular assist devices.
What are we doing to help?
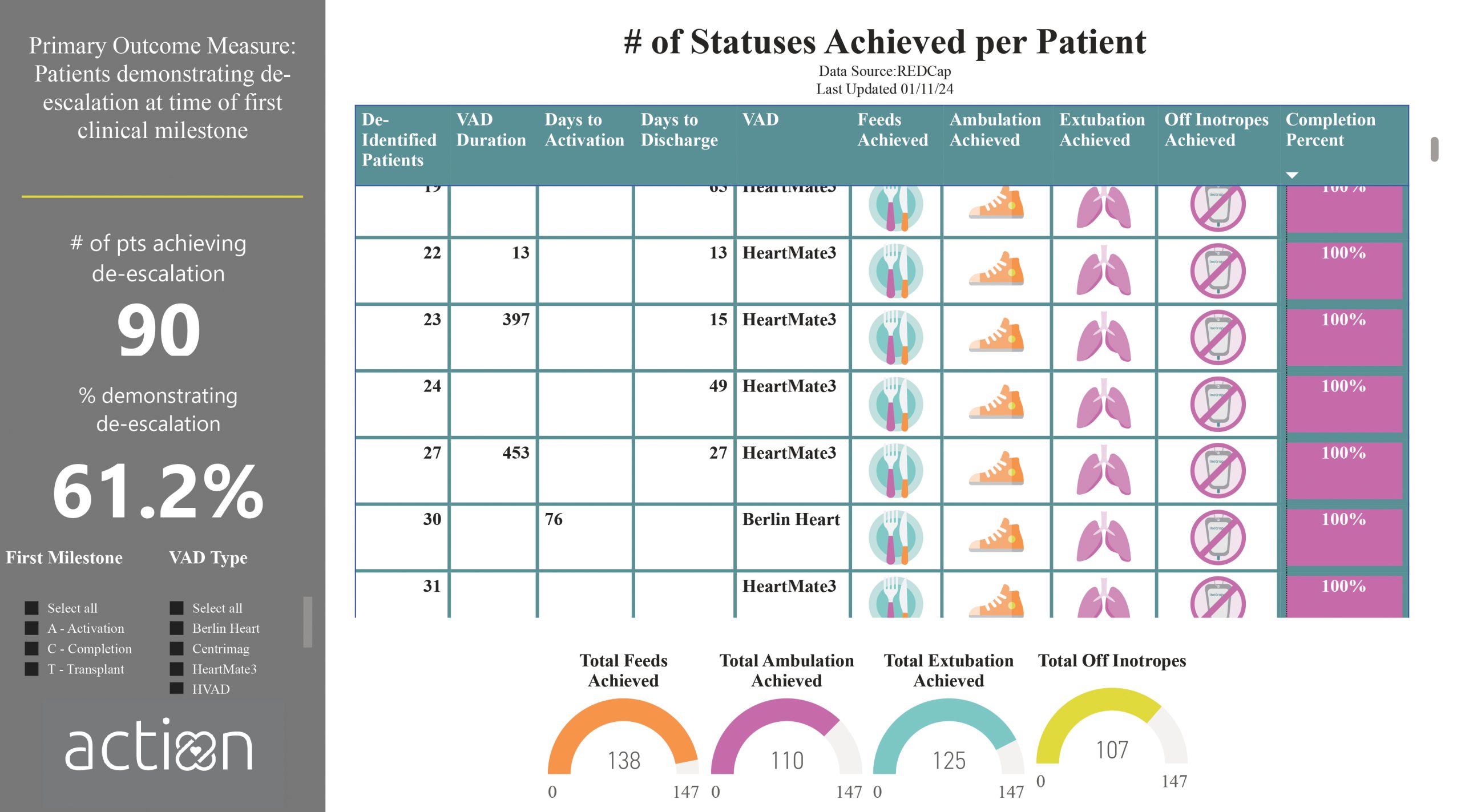
What data do we have?
147 HeartMate 3TM and Berlin Heart patients have been entered in the De-Escalation Project. 90 of the 147 patients achieved de-escalation before either 1. activation for transplant, 2. completing hospital course to discharge, or 3. receiving their transplant. Achieving de-escalation means the patient was extubated, off inotropes, ambulating or age equivalent, and stated feeds. This project is designed to encourage patient stability prior to transplant. It is also an effort to encourage discharge of patients on HeartMate 3TM. Data last updated January 11, 2024